This week, the UK became the latest country in 2015 to suffer suspected MERS cases. Two suspected cases of the Middle Eastern Respiratory Virus Syndrome (MERS) have forced a hospital in Manchester to shut its emergency department. In May, similar events in South Korea (MERS-CoV in Republic of Korea at a glance), mishandled through ignorance and poor infection control within several hospitals, caused multiple outbreaks and a national emergency. Manchester has obviously learnt from their experience.
MERS is the latest virus to act as a global threat, hot on the heels of Ebola and SARS. It emerged in 2012 and has been an ongoing problem spreading to 10 countries in the Middle East, but the Ebola outbreak in West Africa in 2014, replaced it in world headlines (read MERS the next pandemic threat, which appeared also in the Global Health Knowledge Base.
What would happen should MERS ever reach a country with a poor health system?
What do we know about MERS?
Little is yet known of the disease except for its indiscriminate and high mortality rate, particularly among those whose health is already compromised (e.g. diabetes, kidney or lung disease, immunocompromised patients). Health care workers are at risk because human to human transmission requires close contact. 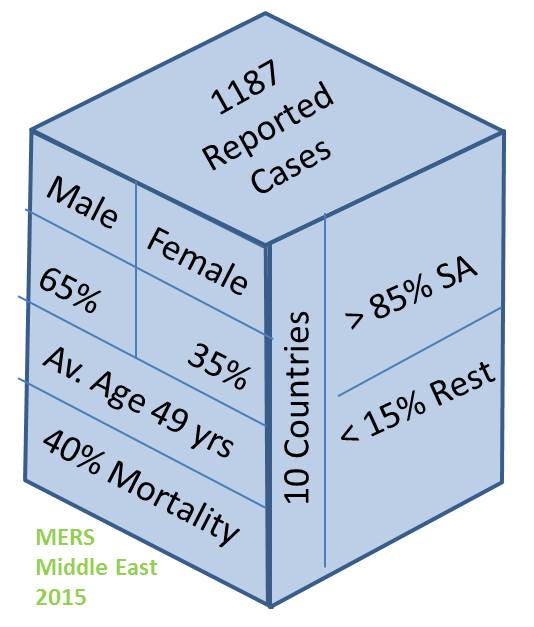
The figure opposite shows the situation in the Middle East in 2015. Note the 40% mortality rate…its as bad as Ebola. Most of the cases occur in Saudi Arabia (SA).
MERS is a zoonotic respiratory disease caused by a beta coronavirus MERS-CoV. Its related to SARS.
MERS and SARS patients experience similar severe acute respiratory illness [fever, cough, and shortness of breath]. SARS was more infectious; MERS is more deadly.

Both SARS and MERS viruses originated with bats, but in the case of MERS it first leapt into camels and they are now considered the animal reservoir not bats. Research identifies camel secretions (saliva, nasal secretions, urine) and camel products (milk, meat) in the Middle East as the source. A higher prevalence of MERS-CoV antibodies has recently been shown in camel herders and slaughterhouse workers, so it is possible that these may be responsible for some human to human transmission.
Early studies indicate that the disease is spread by juvenile camels and that it has been around for a long time (decades) within camel herds. Both community-acquired and hospital-acquired cases have been reported in Middle East but there is no evidence of ongoing community transmission in any country.
The recent flare-up of human cases is linked to transmission in health care settings.
Research is required to answer basic questions such as mode of transmission, natural history, risk factors, pathogenesis, management but also to provide early diagnosis and to explain why the disease has emerged in Middle East and not Africa, where the virus also circulates in camel herds.
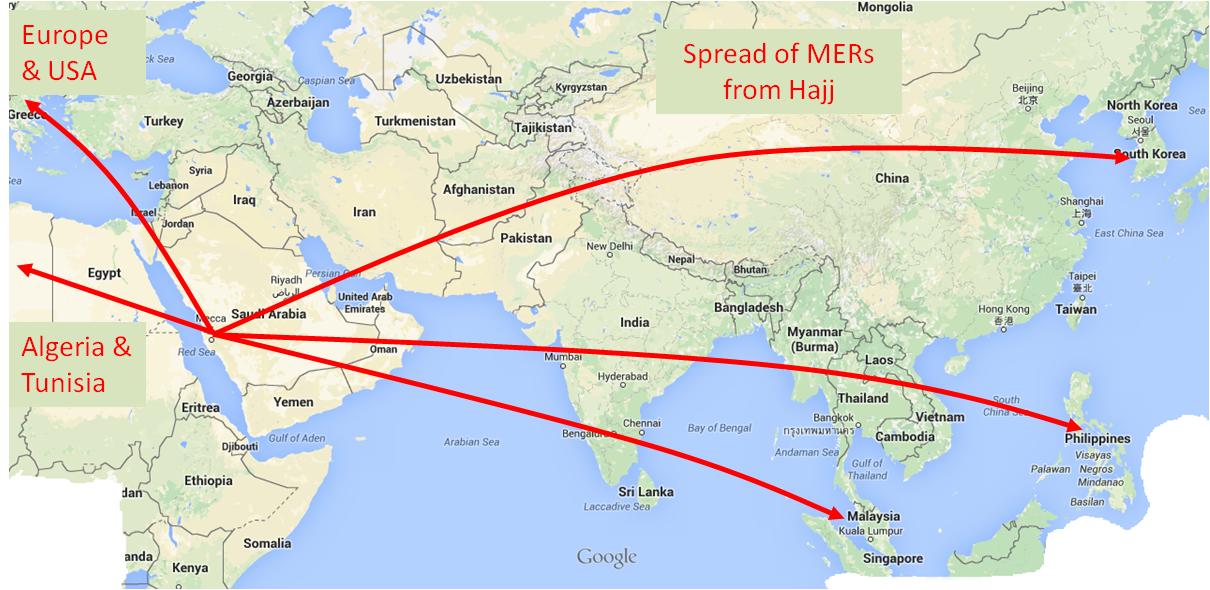
MERS spreads across borders via travel
Travel-related cases have now occurred in Europe, USA, Africa and Asia and all of the index cases have recently returned from the Middle East. Some were health care workers who had been based in the Middle East, but many involved pilgrims who visited Saudi Arabia to perform the Hajj or Umrah. Information within CABI’s Global Health database links the Korean outbreak of MERs to the Hajj, and also identifies another known health risk of this pilgrimage, the risk of meningitis.
Outbreaks outside of the Middle East are always due to nosocomial (hospital-acquired) infections, brought about by lack of awareness of the disease and poor infection control.
Image: Wendie Norris
The recent outbreak in South Korea is a classic case.
It involved a 68 year old man who had recently returned from the Middle East, and sought medical help when he began to experience respiratory symptoms – he was diagnosed as their first MERS patient in May 2015. Significantly, it took visits to 4 different hospitals before he was correctly diagnosed, and this delay lies behind the severity of the outbreak.
By July 3rd, 185 cases had occurred resulting in 33 deaths. One hospital, Samsung Medical Centre (Seoul) was responsible for causing 50% of the cases. Pyeongtaek St. Mary’s Hospital was, in June, reported to be responsible for 41 cases, due to poor ventilation allowing the virus to spread out of the isolation room where the sick man stayed.
Inadequate quarantine and poor public health surveillance also allowed an infected contact (the son of a laboratory-confirmed patient) to travel by air to Hong Kong and then by bus, so spreading the disease to southern China. The contact also contributed to this scenario because he ignored medical advice not to travel. China had to quarantine 64 people.
Now aware of the disease, more effective controls were put in place – the Korean authorities have a programme of contact tracing (up to 2000 so far) and have introduced quarantine and strict hospital infection control – as employed to combat SARS. On July 28th, Korea announced the emergency was over, with a death toll of 36 people.
Where else could MERS strike?
1. Australia for one…It has a large wild camel population (300,000) and apparently also exports them. It also has the bat species which is thought to be the original reservoir for the virus.. Since 2014, CSIRO Animal and Human Health is monitoring the camels and bats for signs of the MERS-CoV, and conducting research to find out more about the disease. 2014 seroepidemiological data suggests that Australian camels are MERS free.
2. Countries with a large Muslim population…This September, any country which has a large Muslim population must be aware of the Hajj, a pilgrimage made by Muslims to Mecca, Saudi Arabia. For instance, over 10,000 Thais are expected to visit Saudi Arabia for the Hajj. The Thai government will be screening ALL those returning with fever monitors and Hajj tour operators are being required to register the names of all their customers. All because of the beta coronavirus MERS.
Importance of Global information to inform Public Health
CABI’s Global Health database addresses public health issues and programmes that cross national boundaries to become regional or global.
As has been said many times, early notice and awareness of a significant infection enables medical and public health officials to get ahead of the disease and introduce measures that prevent disease transmission instead of always playing catch-up to a disease that is no respecter of national borders. Catch-up activities generally take longer, cost much more, and delay the necessary control of the disease with increased deaths. The public, tour operators and airport staff also need to be fully informed so that they apply and obey the correct advice.
Information does indeed save lives.
Sign up to Global Health Knowledge base updates for free at: http://cabiblog.typepad.com/globalhealth/subscribe
This month, August, the topic is antibiotic resistance.
In the News & Research
Juvenile camels 'key source' of Mers
Hajj spurs new Mers outbreak fear
MERS in South Korea and China: a potential outbreak threat?
Did poor ventilation lead to MERS 'superspread' in Korea?
MERS’s best friend is ignorance, so it’s time to wise up
Related articles
Related News & Blogs
3 fast ways to find super-specialized research
We all know that essay deadline dread; you’ve got a rough idea, no clue where to find the right research, and less and less time to get everything (citations included) sorted. Never fear, CABI’s here! In this blog, we share our 3 top tips for finding s…
10 June 2021