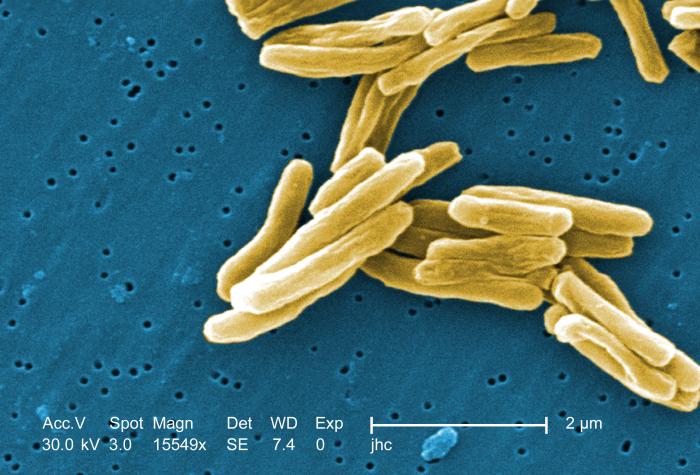
The 1940s saw the beginning of the era of effective drug therapy for TB with the discovery of streptomycin. At the beginning of the 21st century we are seeing its end. Last month doctors in India reported an outbreak of a strain of TB that was termed totally drug resistant. It could be a false alarm because as it turns out the strains were not tested against all known drugs for TB but they were resistant to all 12 of the most common first and second line drugs.
Unfortunately India wasn’t the first place to report totally drug resistance such strains were reported in Italy in 2007 and Iran in 2009. Its presence in India is a concern, say experts because of the large poor population living in crowded conditions and government funded treatment of only simple TB cases.
TB develops drug resistance readily, probably aided by the long treatment times needed. Drug resistant strains followed very soon after the development of the first anti TB drugs and multiple drug resistant (MDR) forms heralded the resurgence of TB globally in the 1980s.
In response the World Health Organization developed the DOTS strategy, where adherence to the drug regime is ensured by observing the patient each time they take a drug dose. But despite this half a million cases of MDR TB occur each year because of poor adherence, poor quality drugs or erratic supply of drugs.
In 2006 the next step on the slippery slope to an incurable TB was the appearance of extremely drug resistant TB in an outbreak in South Africa. This was resistant to first and some secondline drugs.
This increasing drug resistance puts recent progress in decreasing the number of worldwide TB cases in jeopardy.
What can be done? Early diagnosis and testing and a better vaccine would go a long way to getting cases early and giving the right drugs. Treating early and accurately will stop the spread of TB.
TB diagnosis is antiquated – requiring use of microscopy in low resource settings. Matters are complicated by unreliable blood tests on the market which are attractive, quick to do and cheap. WHO issued a warning about those last year.
Progress is being made towards a rapid test. The Xpert MTB/RIF assay is a real-time PCR assay that is fully automated, and that has demonstrated high performance and could be deployed in a range of low- and middle-income settings. The World Health Organization (WHO) has publicly backed it.
World TB day is on 24th March 2012. Join the campaign against this disease of poverty here.
CABI is publishing a book about tuberculosis this year: Tuberculosis diagnosis and treatment.
See Global Health Knowledge Base for access to Global Health abstracts on tuberculosis
Photo credit: Janice Haney Carr
Related News & Blogs
Global health security, collaborating to stop epidemics
Global health security is defined as stopping the spread of infectious diseases and drug resistance across borders. Its a concept being put into action by the Global Health Security Agenda, a commitment by over 50 member countries, NGOs and international donors to assess and improve health systems to stop outbreaks, as happened with Ebola in West Africa, turning into epidemics. We review progress on malaria and on neglected tropical diseases as detailed in the 2017 annual report of UK’s All-Party Parliamentary Group for Malaria and Neglected Tropical Diseases, entitled “Global Britain in the Fight against Malaria and Neglected Tropical Diseases”.
5 February 2018